Predictive Value of Electroencephalography for Seizure Outcome Following Corpus Callosotomy in Children
Article information
Abstract
Background and Purpose:
This study aimed to determine whether preoperative or postoperative electroencephalography (EEG) can predict surgical outcome for corpus callosotomy.
Methods:
We retrospectively reviewed the medical records of 16 patients enrolled. We compared postoperative seizure outcome according to seizure type, preoperative interictal EEG, preoperative ictal EEG, and postoperative interictal EEG. Seizure outcome was classified according to postoperative seizure reduction, i.e., seizure free, >90%, 50–90%, <50%, and no change or worsened. A seizure reduction of 50% or more was judged as a “favorable outcome”.
Results:
Most patients showed a favorable outcome (12 patients, 75%) and two patients became seizure free (13%). Atonic seizure was most responsive to corpus callosotomy. Preoperative interictal epileptiform discharge had 3 patterns; bilateral independent, generalized, and combination of independent and generalized. None of the preoperative interictal epileptiform discharge (EDs) had significant correlation with seizure outcome. The preoperative ictal rhythm did not predict seizure outcome. However disappearance of generalized EDs on postoperative EEG was correlated with favorable seizure outcome.
Conclusions:
The presence of generalized EDs on postoperative interictal EEG predicted seizure outcome, whereas preoperative EEG did not.
Introduction
It is known that the corpus callosum play a principal role in interhemispheric synchronization and propagation of epileptic discharge.1–3 Based on this transfer theory, the corpus callosotomy (CC) has been preformed to treat the intractable generalized seizures.4–11 Many clinical series had accumulated and gained some general acceptance. Patients seldom become seizure-free following CC but had favorable outcome. While drop attacks (atonic seizures) and secondarily generalized tonic-clonic seizures respond remarkably, partial seizures might be even worse after CC.4–13 However controversy still exists regarding the surgical extent, patient selection and predictive factors despite evolution in technique of CC. Especially the relationship between EEG pattern and the seizure outcome is not entirely understood and little is known in children.3,14–20 This study aimed to analyze the EEG pattern and attempted to determine whether the preoperative or postoperative EEG pattern can predict the surgical outcome in children.
Methods
Selection of patients
A retrospective analysis was made of children who underwent CC between July 1995 and July 2009 at Seoul National University Children’s Hospital. Sixteen patients were identified who met the following criteria; (1) uncontrolled generalized seizures despite use of appropriate anticonvulsants for at least 1 year, (2) seizures were disabling to interfere with daily living or significant in character, and (3) the patients without discrete resectable focus. This study was approved by institutional review board.
Preoperative evaluations
All patients underwent MR imaging studies, scalp EEGs, and neuropsychological testing prior to CC. Long-term video EEG monitoring was performed to confirm the seizure types and assess the possibility for potential respective surgery in most cases.
Seizure types
The nomenclature for seizure was employed by the Commission on the Classification of International League Against Epilepsy. Seizure types in this study included atonic seizure, myoclonic seizure, generalized tonic-clonic seizure (GTCS), atypical absences, complex partial seizure (CPS), and simple partial seizure (SPS). Based on seizure type, patients were divided into two groups: one group with generalized seizures only and another group with both generalized and focal seizures.
Extent of callosotomy
The extent of CC consisted of two categories. In the past, the anterior 2/3 CC (sparing splenium of the corpus callosum) was more preferred to decrease the incidence of the disconnection syndrome. With the evolution of CC, our preliminary experience has suggested that younger patients can tolerate a one-staged complete CC with little complications. Recently complete CC has been performed as the initial procedure.
Postoperative seizure outcome
An assessment of surgical outcome was made more than 6 month after CC. The clinical responses were grouped into the following 5 grades on basis of postoperative seizure reduction: seizure-free, >90%, 50–90%, <50%, and no change or worsened. A seizure reduction of 50% or more was judged as “favorable outcome”.
Statistical analysis comparing outcomes was performed utilizing Mann-Whitney U test and Kruskall-Wallis test. Changes were considered statistically significant when the p-value was <0.05.
Analysis of EEG
The digital EEGs were recorded 19 scalp electrodes placed on according to the international 10–20 system. Epileptic discharges (EDs) were classified as focal (confined to a single lobe), unilateral (confined to a hemisphere), bilaterally independent, bilaterally synchronous, and generalized bursts. Bilaterally synchronous EDs were regarded as generalized EDs. Evaluation was done before operation and more than 1 month after CC.
Results
Characteristics of patients
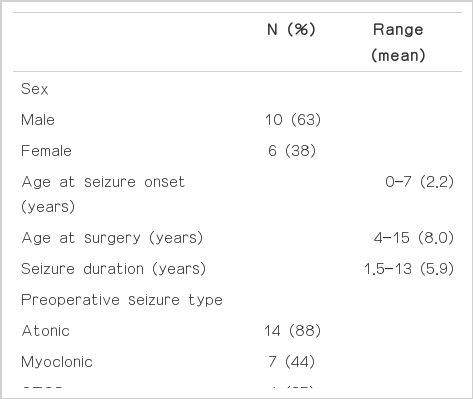
The clinical data of the 16 children is provided in Table 1. The mean age of seizure onset was 2.2 years (range 2 days to 7 years), the mean age at surgery was 8 years (range 4 to 15 years), and the mean duration of epilepsy prior to CC was 5.9 years (range 1.5–13 years). Most of them had more than one type of seizures. Atonic seizures was the most and atypical absence the least. Seven patients had spasms previously.
Preoperative MR imaging revealed normal in 10 patients and abnormal findings included hypoxic ischemic encephalopathy, nonspecific diffuse brain atrophy, Dandy-Walker variant and multifocal pachygyria. All of the patients showed mild to severe mental retardation.
Anterior 2/3 CC was performed in 5 patients and complete CC in 11. Three patients of 11 complete CC had 2-staged CC due to ineffective seizure control after anterior 2/3 CC.
Seizure outcome
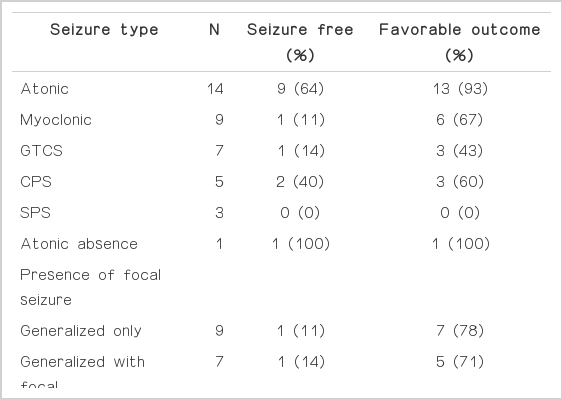
For the overall seizure outcome, majority of patients achieved favorable outcome (12 patients, 75%) and 2 patients became seizure-free (13%). Seizure outcome for each seizure type is shown in Table 2. Atonic seizure and atypical absence were the best responsive to CC whereas SPS improved least. Especially for the atonic seizure, nine patients became seizure-free and 13 patients showed favorable outcome. There was no change of atonic seizure in one patient who was performed anterior 2/3 CC.
All patients experienced either generalized seizures only or mixed seizures (both generalized and focal seizures). As shown in Table 2, there was no statistically no difference in seizure-free rate and favorable outcome (p>0.05).
Four patients developed new types of seizure after CC. SPS occurred in 3 (19%) patients, myoclonic seizure in 2 (13%), and CPS in 1 (7%). Although 3 patients showed favorable outcome, no one achieved seizure-free.
Preoperative interictal EEG
The correlations between preoperative EEG pattern and seizure outcome are described at Table 3. In half of patients showed abnormal background activity such as diffuse delta slowing, focal slowing, and poor regulation of posterior rhythm. There was no significant difference in seizure-free rate and favorable outcome (p>0.05).
The patterns of preoperative interictal EDs were divided into 3 groups. One group showed bilaterally independent EDs only (3 patients, 19%), another generalized EDs only (3 patients, 19%), the other combinations of bilaterally independent EDs and generalized EDs (10 patients, 63%). There were no statistically no difference in seizure-free rate and favorable outcome among 3 groups (p>0.05). Comparing generalized EDs only group with other groups, the absence of focal EDs were not correlated with better seizure outcome.
Preoperative ictal EEG
Eleven patients underwent long-term video EEG monitoring to identify seizure type. Ictal rhythm had 3 patterns; one was spike discharges (spike, polyspike, or spike-and-wave discharges), another diffusely increased delta activity, and the other combination of spike and delta activity. There was no significant difference in surgical outcome among 3 patterns (p>0.05).
Sometimes initial ictal rhythm was followed by diffuse background attenuation but this finding was not related to the seizure outcome (p>0.05).
Postoperative interictal EEG
The correlations between preoperative EEG pattern and seizure outcome are described at Table 4. Generalized EDs were disappeared in some patients after CC. There was no newly developed generalized EDs. The presence of generalized EDs after callosotomy had significant correlation with favorable seizure outcome (p=0.01) though it did not affect seizure-free rate. Likewise the disappearance of previously present generalized EDs was significantly associated with a favorable outcome (p=0.004).
EEG changes related with extent of callosotomy
It is generally accepted that anterior callosotomy is less effective than complete callosotomy as to seizure reduction. To avoid confounding, the persistence of generalized EDs was evaluated according to the extent of callosotomy respectively (Data not shown). Between anterior callosotomy and complete callosotomy, there was no significant difference in the presence of generalized EDs preoperatively and postoperatively.
Discussion
Since its introduction by Van Wagenen and Herren in 1940, CC has been widely used to treat medically intractable epilepsy not amenable to focal resection.21 A significant number of clinical studies have shown different results. These discrepancies are mainly caused by variability of patient selection, varying extent of callosal resection, target seizure type, different outcome measures and definition of successful outcome.
Most studies have shown a 50% or greater reduction in seizure frequency regardless of the extent of callosal resection. In our study, the effect of CC for seizure reduction was not dissimilar to previous reports.6,10–12,19,22–27 Two of 16 patients (13%) became seizure free and 12 patients (75%) achieved a favorable outcome. Atonic seizures were the most responsive to CC. This rate is as high as that reported in other series.
The correlation of seizure outcomes as to EEG pattern has not been fully established. The current study analyzed preoperative and postoperative EEG, respectively.
In some studies, preoperative interictal EEG has had prognostic significance. Bilaterally independent spikes on interictal EEG were associated with poor outcome.6 The presence of slow spike-and-wave of the interictal EEG was of borderline significance for better seizure outcome in one study.9 In contrast, some studies found no relationship between preoperative interictal EEG and outcome.28,29 According to our results, seizure outcome was not predicted neither by abnormal background activity nor generalized EDs on preoperative interictal EEG.
There were variable results as to relationship between ictal rhythm and prognosis. In one report ictal EEG was important predictive factor. The ictal rhythm including generalized slow spike-and-wave, electrodecrement, or nonevolving low amplitude fast activity showed more favorable outcome than others.19 Another studies found that total amount of EDs on ictal EEG was not correlated with seizure outcome.15,16 The data observed in our patients ndicated that ictal rhythm was not predictive factor. Besides initial ictal rhythm, we attempts to determine whether the following diffuse attenuation can predict outcome. We speculated that the presence of diffuse attenuation (desynchronization) would be related with poor outcome because of the possibility of epileptogenesis via other pathways except corpus callosum. Contrary to our expectation, the presence of diffuse attenuation was unrelated with seizure outcome.
Previous reports for EEG changes following CC consist of a marked disruption of preoperatively present bilateral synchrony, localization of EDs, and the appearance of bilaterally independent spike-and-wave.15–17,30 In this study, the diminishment or absence of generalized EDs on the postoperative interictal EEG was a good prognostic sign. These results correspond with the earlier studies.3,11,16,24,26
In summary, the present study indicated that the presence of generalized EDs after callosotomy would predict the seizure outcome whereas preoperative EEG not.