In patients with no abnormal findings on a thorough vestibular evaluation, spontaneous recurrent vertigo can be attributed to various conditions, including vascular vertigo, vestibular epilepsy, and psychogenic dizziness.1 Vascular vertigo can be identified with an assessment of the migraine history, diagnostic images, vascular risk factors, and specific evoked positions (i.e., rotatory vertebral artery syndrome). Vestibular epilepsy is confirmed by the incidence of vertigo attacks associated with appropriate changes on electroencephalography (EEG).1 Psychogenic dizziness may also be considered when the patient’s dizziness cannot be attributed to other vestibular disorders.2 We report a patient with psychogenic dizziness that mimicked vestibular epilepsy.
Case Report
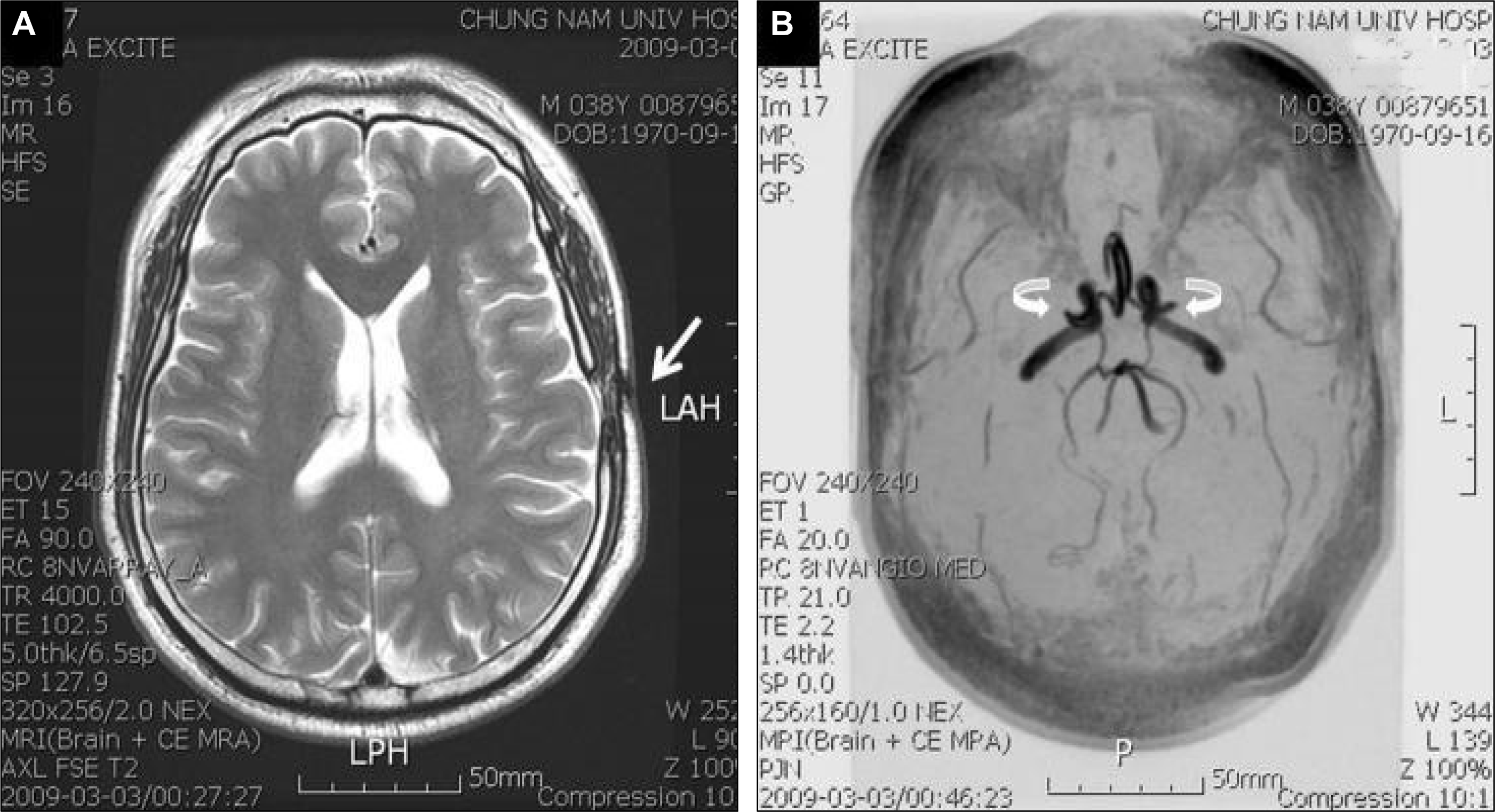
A 28-year-old man presented to our clinic three days after his first episode of vertigo. The patient was suffering from frequent episodes of severe spinning vertigo with mild nausea; each episode lasted for a few minutes. The patient complained of a severe whirling sensation with a clockwise direction during the ictus, and experienced a dull headache after the ictus. The patient reported that he did not suffer from agoraphobia, panic symptoms, or any recent stressful conditions. Nor was the ictus accompanied by ear symptoms, such as tinnitus, hearing loss, or aural fullness, and there were no other symptoms, such as paresthesia, motor deficit, or visual disturbances, including field defect, metamorphopsia, or color change. His symptom was not predictable and occurred without any position change. The patient did not lose consciousness during the onset of the symptom, and his family members had not witnessed any eyeball deviation or head turning during the episodes. The patient had no history of motion sickness or migraine. However, he had undergone an operation in the left cerebral hemisphere for the treatment of Moyamoya disease (encephaloduroarteriosynangiosis, EDAS) 3 years ago. Brain MRI revealed the presence of an osteoplastic craniotomy scar in the left lateral convexity (Figure 1). No nystagmus was observed and his symptoms were not evoked by the hyperventilation maneuver. The patient showed bilaterally symmetrical saccade and smooth pursuit. A cerebellar function test was normal and a caloric test and audiometry showed normal responses. We assumed that the ictus was a manifestation of vestibular epilepsy. Therefore, the patient was admitted to the Epilepsy Monitoring Unit (EMU). He was monitored continuously for 24 hours a day with video and computerized EEG equipment. However, the episodes of vertigo were not accompanied by any significant EEG changes, such as sharp waves and spikes. Therefore, we suspected that the episodes might be psychogenic dizziness. The patient was responsive to benzodiazepine medication and psychological encouragement.
Discussion
We have reported a case of psychogenic dizziness mimicking vestibular epilepsy. Psychogenic dizziness is generally characterized by a vague giddiness or a dissociated sensation that is attributable to the impaired central integration of the sensory and motor signals in patients with acute and chronic anxiety.2 Because there is an associated risk of ignoring important underlying disorders, the clinical diagnosis of this condition should be made with caution. Generally, patients with psychogenic dizziness may complain of a spinning sensation inside their heads or they may experience a swaying sensation when standing still.3 However, our patient complained of a severe whirling sensation with clockwise directionality. He reported suffering no other panic symptoms or anxiety.
The cortical injury to the patient’s left hemisphere, caused by an EDAS operation, could have evoked his recurrent vertiginous attacks. Although there is no primary vestibular cortex in humans, the cortical vestibular function is performed via a network of multisensory visual-vestibular-somatosensory pathways and is distributed over several separate and distinct areas of the temporoparietal region.1 When vestibular seizures arise in different areas, there may be differences in the sensorimotor symptomatology with regard to the apparent rotation or tilt, the head and body deviation, or epileptic nystagmus.4 However, in our patient, there were no changes on EEG during the vertigo attacks during 24-hour EMU monitoring and a vestibular evaluation produced no abnormal findings. The patient’s recurrent episodes of vertigo were alleviated by the management of psychogenic dizziness. Therefore, we conclude that psychogenic dizziness may also manifest as recurrent whirling vertigo with unilateral directionality.