Introduction
Anti-NMDA receptor antibody encephalitis is a recently recognized autoimmune encephalitis characterized by a prodromal phase of nonspecific illness with fever resembling viral disease, followed by memory loss, psychiatric features, seizures, disturbed consciousness, abnormal movements and autonomic imbalance. In 2008, Dalmau et al. reported a case series of 100 patients with anti-NMDA receptor antibody encephalitis. Various types of seizures occurred in 76%.1 Among them, 45% were generalized tonic clonic seizures and 10% were partial complex seizures. Status epilepticus was reported in only 6%, but details were not specified. Electroencephalography (EEG) was reported to show generalized or fronto-temporal delta or theta slowing in 77%, and epileptic activity in 23% of patients.1 There have been only few reports of non-convulsive status epilepticus (NCSE) related to anti-NMDA receptor antibody encephalitis.2–5
We report a case of anti-NMDA receptor antibody encephalitis with confusion, poor-orientation and unilateral rigidity, which correlated with unilateral rhythmic delta activity, and which was finally proven to be NCSE.
Case Report
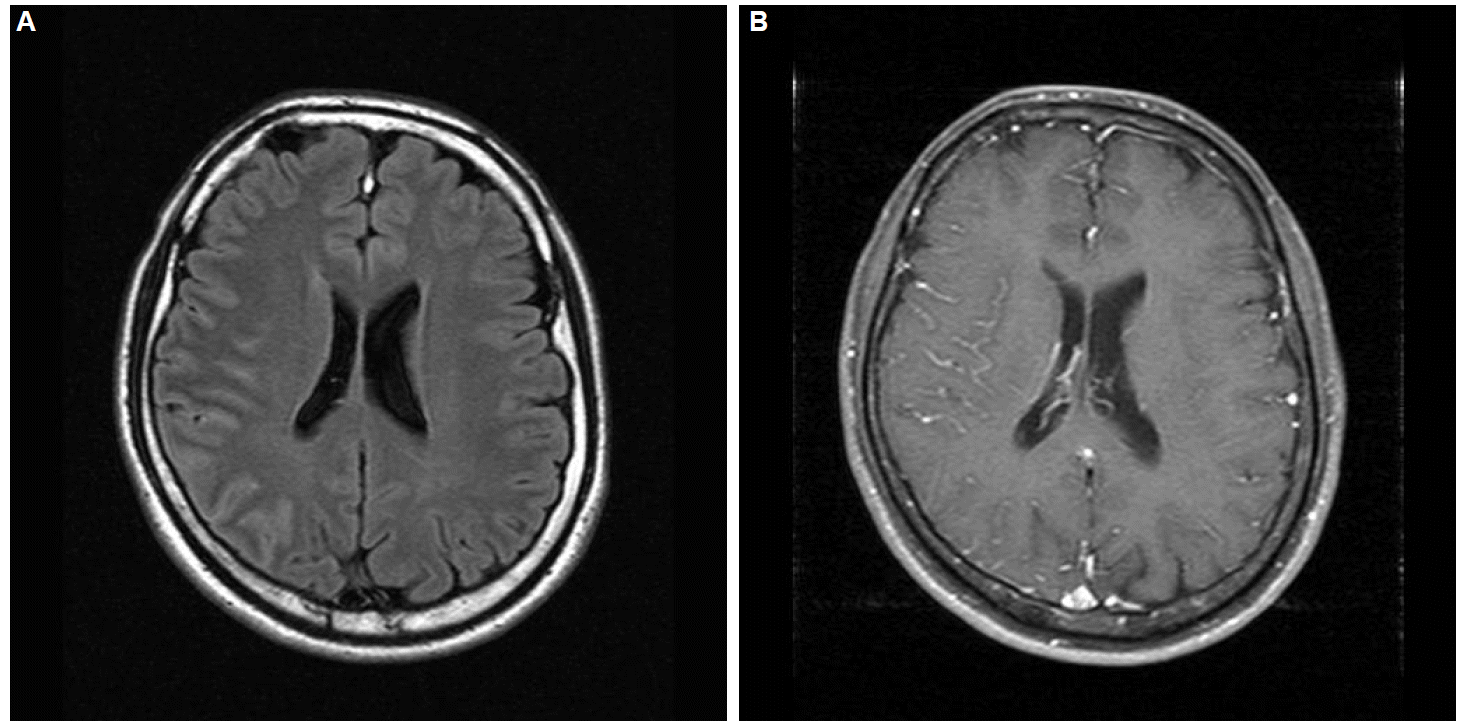
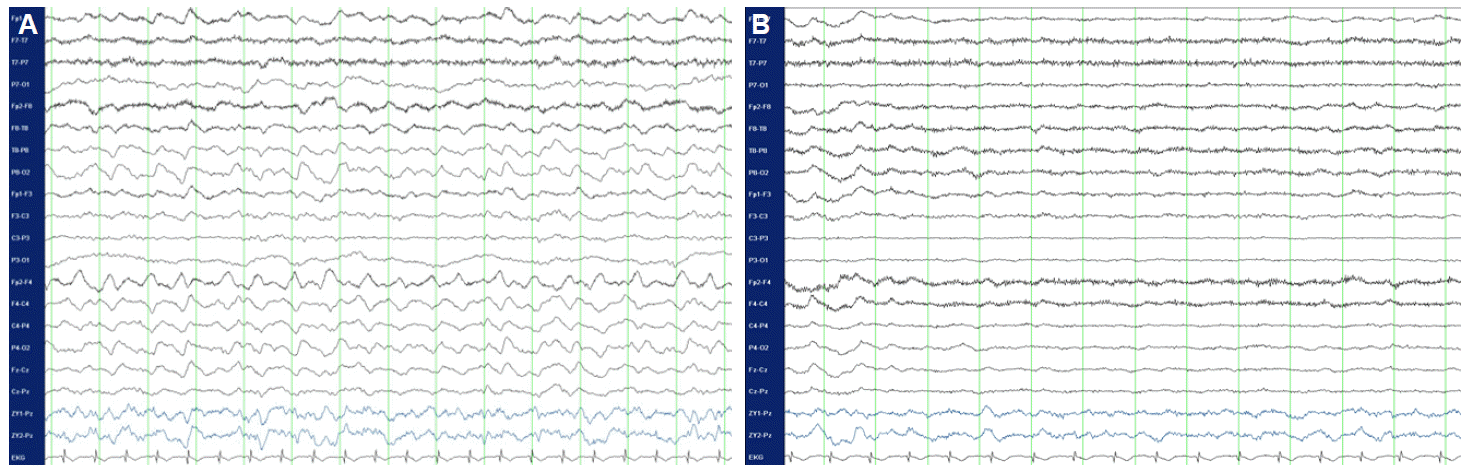
A 34-year-old previously healthy man initially complained of nonspecific headaches and mild fever for a month. Subsequently, he began to show intermittent confusional episodes. He sometimes had incoherent and meaningless speech, followed by complete recovery. He was admitted to our hospital for recurrent confusional episodes. On neurologic exam, the patient was alert but poorly responsive. Pathologic reflexes were negative, but the muscle tone of the left arm and leg were slightly increased. Analysis of cerebrospinal fluid (CSF) identified 91 white blood cells/mL (80% lymphocytes) and normal level of protein and glucose. Laboratory tests including routine chemistry and electrolytes revealed no abnormalities. Brain magnetic resonance imaging showed abnormally high signal intensities in the right fronto-parietal gyri on FLAIR image. Gadolinium-enhanced T1-weighted images showed diffuse leptomeningeal enhancement in the righthemisphere (Fig. 1). Under an initial differential diagnosis of viral meningoencephalitis, intravenous acyclovir was begun. Twenty four hour video EEG monitoring was started due to fluctuating consciousness. EEG showed rhythmic delta waves in the right hemisphere. After injection of lorazepam, delta waves on EEG disappeared and clinical symptoms improved, which was suggestive of NCSE (Fig. 2). Phenytoin (300 mg/day), valproate (1,000 mg/day), topiramate (400 mg/day) and levetiracetam (2,000 mg/day) were used to control the seizure activity. Anti-NMDA antibody test was positive in the serum and CSF. Initially, he was treated with pulse dose of methyl-prednisolone (1g for 3 days and 500 mg for 2 days) and steroids were tapered by dexamethasone (12 mg for 7 days, 9 mg for 3 days, 6 mg for 3 days and 3 mg for 3days). Neck, chest, abdomen and pelvic computed tomography, and whole body positron emission tomography revealed no evidence of malignancy. His mental state markedly improved after antiepileptic medication but mild confusion lasted more than 2 weeks, which gradually disappeared with steroid therapy. After discharge, antiepileptic drugs and steroids were slowly tapered for 4 months. He returned to his normal life without any medication.
Discussion
The present case describes a young man with anti-NMDA receptor antibody encephalitis who showed intermittent confusion and decreased responsiveness associated with unilateral NCSE.
Dalmau et al. reported various types of seizure in 76% of anti-NMDA antibody encephalitis.1 Status epilepticus was reported in 6% of patients. We recognized that our patient’s unilateral delta activity might be ictal pattern of NCSE due to the improvement of EEG and clinical status after intravenous lorazepam injection.6 There have been four case reports of non-convulsive status epilepticus due to anti-NMDA receptor antibody encephalitis. These cases showed unresponsiveness and related various EEG abnormalities. One case showed focal 12–13 Hz epileptiform discharges,2 two cases showed generalized theta to delta activity,3,4 and the other case showed unilateral 1 Hz rhythmic right hemispheric delta activities as NCSE pattern, similar to our case.5
Titulaer et al reported that adult men more often (27%) presented with seizure than adult woman (11%, p = 0.007), who usually presented with abnormal behavior and psychiatric symptoms.7 The authors suggested hormonal factors and selection bias for the different sex-related symptom presentation.
In conclusion, our case suggests that suspicion of the diagnosis of anti-NMDA receptor encephalitis in adult men with unexplained mental status is needed. Furthermore, EEG monitoring may be useful in cases of suspected anti-NMDA receptor encephalitis even in the absence of overt seizures, given the possibility of NCSE.