Introduction
Epilepsy impacts the brain, and is associated with cognitive dysfunction and behavior disorder, which can affect quality of life, especially during the developmental period.1–3 Early onset epilepsy, particularly in those less than 3 years old, and uncontrolled seizures are associated with poor cognitive function later in life.4
Currently, more than 20 different antiepileptic drugs (AED) exist for the treatment of epilepsy. However, 30% of patients with epilepsy continue to have seizures.5–7 Many new medications have been approved in the past two decades, but these have not reduced the proportion of patients with intractable epilepsy.5 Recently, cannabis has attracted attention as a potential treatment of epilepsy.7 Cannabis was used to treat epilepsy in Sumeria as early as 1800 BCE.7,8 In the late 19th century, English neurologists also used cannabis for the treatment of epilepsy.9–11 More recently, some states in America have approved medical marijuana for the treatment of epilepsy. Moreover, since 2013, the effects of cannabidiol (CBD) in the treatment of epilepsy have been studied at 10 epilepsy centers using Epidiolex, a purified cannabis containing 99% CBD and less than 0.10% tetrahydrocannabinol (THC). (GW Pharmaceuticals, Sativex, London, UK).
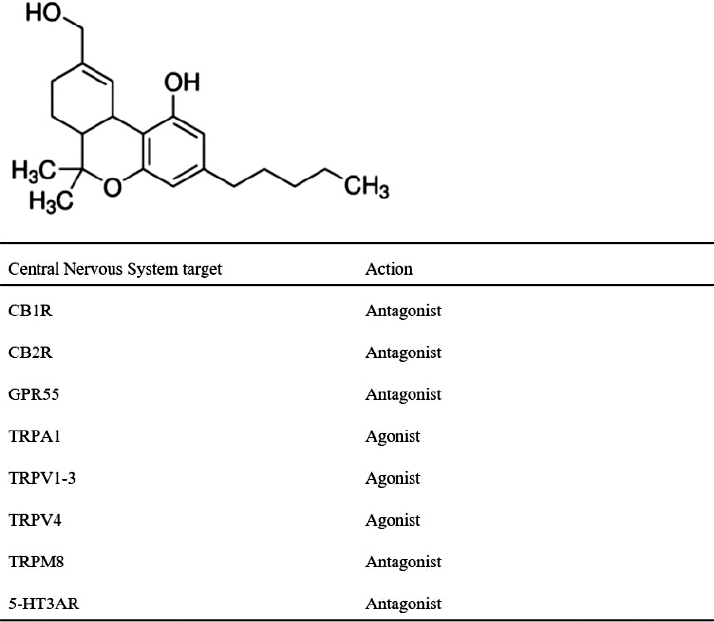
Cannabis contains more than 545 distinct compounds, the most abundant of which are cannabinoids.12 The most important neuro-active components of cannabis are CBD and Δ9-THC. THC binds to G-protein-coupled cell membrane receptors, including the cannabinoid receptor type 1 (CB1R), which is found primarily in the brain, but is also present in peripheral tissues, and the cannabinoid receptor type 2 (CB2R), which is located mainly in immune and hematopoietic cells. THC binds CB1R in inhibitory gamma-aminobutyric acid-ergic and excitatory glutamatergic neurons.13,14 These interactions are the pathways by which cannabis exerts its psychoactive function. However, CBD is an antagonist to CB1R and CB2R.15 Some animal studies show that CB1R antagonists can reduce the threshold of seizures.16 This suggests that CBD has another mechanism by which it can control seizures. Indeed, CBD acts via multiple mechanisms (Fig. 1).7,14,15 These include effects on transient receptor potential ation channels at a low level,17 and antagonistic functions at G-protein-coupled receptor 55, by which it can decrease presynaptic glutamate release.18 However, the mechanisms underlying the anti-epileptic effects of CBD are not well defined.
CBD is metabolized by the liver, and it can inhibit cytochrome P (CYP) 450, especially CYP 2C and CYP 3A, which aids metabolism of several AED.19,20 Therefore, if a patient with epilepsy takes CBD with an enzyme-inducing AED, such as carbamazepine or phenytoin, the AED can reduce serum CBD levels. Whereas, if the patient takes clobazam (CLB) with CBD, CBD can raise the serum level of nor-oclobazam, the active metabolite of CLB.21 The half-life of CBD in humans is estimated to be between 18 and 32 hours.22
Here, we review recent trials that have investigated the use of CBD as a treatment for epilepsy and highlight key issues for future research.
Trial dosages of CBD
In many studies, CBD was added to a baseline AED at an initial dose of 2–5 mg/kg/day divided into two doses. CBD was up-titrated by 2–5 mg/kg once a week until intolerance or to reach a maximal dose of 25 mg/kg/day. Some studies increased the does to 50 mg/kg/day, as allowed by the US Food and Drug Administration. The average of dose of CBD was 200–300 mg/day.7
Clinical trials of CBD to treat epilepsy
Some U.S. states now allow the use of cannabis for medical treatment. Many patients with epilepsy have wanted to try cannabis as a treatment even though preclinical and clinical evidence is limited. As mentioned above, several clinical studies have investigated CBD after the late 19th century. Recent studies have shown an effect of CBD in treating epilepsy (Table 1). They suggest that CBD can reduce the frequency of seizures, reducing monthly frequency in most types of seizures. Many studies have included a significant number of patients with Dravet syndrome (DS) and Lennox-Gastaut syndrome (LGS), and have observed reduced seizures as an effect of CBD.
Between 2014 and 2015, Devinsky et al.23 conducted a prospective, open-label, and expanded trial at 11 epilepsy centers in America. They enrolled 214 patients in the study, of which 137 (64%) were included in an efficacy analysis group and 162 (76%) were included in a safety analysis group. They observed enrolled patients for 12 weeks. This study reported a decrease of 34.6% in the median change of total seizures after 12 weeks’ treatment with CBD. It also showed a decrease of 55% in focal seizures and 54.3% in atonic seizures. They observed a decrease of 36.5% and 16% in tonic seizures and tonic-clonic seizures, respectively. Overall, the median monthly frequency of motor seizures decreased by 47%.
This open-label trial enrolled a large portion of patients with DS (n = 32) or LGS (n = 30). In the case of DS, 16 patients (50%) showed a reduction in motor seizures of more than 50%, and one patient (3%) was free from motor seizures during the 12 weeks of treatment. They reported a median change of −69.2% in monthly tonic seizures (n = 6) and a median change of −46.7% in monthly tonic-clonic seizures (n = 29). Non-motor-focal seizures (n = 10) were observed to show a median reduction of 83.3%. Among patients with LGS (n = 30), 11 (37%) showed a decrease in seizures of more than 50%, but none were seizure free during treatment. The percentage change in monthly seizures for all seizure types was −35.5%. The median change for atonic seizures (n = 14) was −68.8%. In patients with tonic seizures (n = 21), there was a median reduction of 44.0%. However, there was no change in tonic-clonic seizures (n = 16).
Infantile spasm (IS) is another epileptic encephalopathy in need of an effective treatment. In 2014, Hussain et al. conducted a survey about CBD exposure,24 which included patients with IS and LGS. Although this study had several limitations, it supported the possibility that CBD could effectively treat IS and LGS.
Hess et al. studied the efficacy of CBD for refractory epilepsy in tuberous sclerosis complex (TSC).25 They enrolled 18 patients with epilepsy and TSC between 2014 and 2015, and treated them for 6–12 months with CBD. In total, 14 patients (77%) had a mutation, half of whom had a TSC1 mutation and the other half of whom had a TSC2 mutation. At baseline, 72% of patients had shown one or more type of seizure.25 In this study, the median total weekly seizure frequency reduced by 32% after 2 months and 55% after 6 months. At study completion after 12 months of treatment, the seizure frequency was decreased to 63%. Regarding the CBD effect on each type of seizure, epileptic spasms and atonic seizures showed the greatest response. The responder rate of tonic-clonic seizures was 66.7% after 3 months’ treatment. The rates of complex partial seizures and complex partial seizures with secondary generalization were 53.8% and 50% after 3 months’ treatment, respectively. This study was limited by a small sample size, as well as an uncontrolled and unblinded design, but suggests a potential effect of CBD in TSC.
Reported adverse effects
In previous studies, the most common adverse effect of CBD was drowsiness. Most reported adverse effects were mild, for example diarrhea, fatigue, and decreased appetite. Nonetheless, some more serious effects, including status epilepticus, have been reported.
Devinsky et al. reported adverse events in 128 (79%) of 162 recruited patients.23 Most of these adverse effects were mild or moderate, and transient. Critical adverse effects considered to be caused by CBD were observed in 20 patients (12%).23 The most common adverse event was somnolence, while status epilepticus was the most severe and required urgent treatment (Table 2). It is interesting that CBD had this severe adverse effect, status epilepticus, because animal studies have not shown any proconvulsant effects of CBD.9,26 Devinsky et al. also reported thrombocytopenia in 5 patients (3%), but there were no clinical changes in white or red blood cells. CBD also did not affect renal function. Ten patients (6%) showed elevated liver enzymes and this elevation was significant in one patient (< 1%). The authors did not find any relationship between status epilepticus and reduced doses of AED or CBD. Four patients stopped CBD treatment before the end of 12 weeks because of a worsening of seizures or poor efficacy.
Discussion
Most studies suggest anticonvulsant effects of CBD, and consider most adverse effects to be mild. As such, we might expect CBD to show efficacy and safety in the treatment of epilepsy. However, there is potential placebo effects biasing these results. In a study by Purcarin et al.,27 the placebo effect rate for the reduction of median seizure frequency was 10% and the placebo effect was 19% in cases in which seizure frequency decreased by 50% or more. According to the study of Zaccara et al.,28 greater placebo effects were observed in pediatric patients with epilepsy treated with CBD than were in adults. A placebo effect is a concern for many studies because of the media attention attracted by CBD, which is likely to interest parents of children with epilepsy. In most studies, seizure frequency was used as an indicator of efficacy. However, to increase the accuracy of proposed effects, data from clinical tests, such as electroencephalograms, are necessary.
Due to the absence of a control group in previous studies, the adverse reactions to CBD may also have resulted from a bias. For example, many studies reported gastrointestinal problems, such as diarrhea and decreased appetite. However, CBD is usually in the form of oil, which may have precipitated these effects. Therefore, the adverse effects should be reviewed. Furthermore, other adverse effects, such as drowsiness, thrombocytopenia, and elevated liver enzymes, also require more research to exclude the potential influence of AEDs, such as clobazam and valproate. Status epilepticus, the most common severe adverse effect, was not clearly related to CBD because a large proportion of the enrolled patients had refractory epilepsy syndromes, such as LGS, DS and IS.
CBD not only has potential therapeutic effects on epilepsy, but may also be effective in treating various other neurological problems.9 In one study, CBD showed antioxidant, anti-inflammatory, neuroproliferative, and remyelinating effects.29 While cannabinoid receptor agonists can reduce hypoxic-ischemic brain injury,29 lasting overactivation of CB1R can have potential disadvantages. However, CBD does not have agonist effects on CB1R and so can be an alternative treatment.30 Furthermore, CB2R is one of the primary receptors affected by CBD action in the immature brain.30,31 In animal studies, CBD has been shown to reduce injury to neurons and astrocytes due to hypoxia.31,32 This suggests that neonatal hypoxic ischemic encephalopathy could be treated with CBD. This should be a focus of future studies.
One of the most significant limitations of previous studies is their open-label, uncontrolled design and the use surveys. Future research should use blinded, randomized, controlled trials to confirm the efficacy and adverse effects without bias. Currently, many studies are limited to epilepsy, mainly enrolling patients with LGS and DS. Further studies of other epilepsy syndromes are also needed in future.
It must be borne in mind that CBD is still illegal in many contexts. However, it has the potential to treat various neurological problems, including epilepsy. We should seek to clarify the mechanisms underlying the antiepileptic effects of CBD and its efficacy for other neurologic problems. Furthermore, drug-drug interactions with AEDs require further research. Previous studies have determined exact therapeutic drug levels of CBD in the blood. Therefore, this also needs to be clarified to enable effective treatment of epilepsy with CBD.