Introduction
Severe acute respiratory distress syndrome coronavirus-2 emerged in late 2019 and vaccines had been administered worldwide. Research on complications of coronavirus disease 2019 (COVID-19) vaccination is ongoing. Several neurologic complications include encephalitis had been reported, but the case of N-methyl-D-aspartate (NMDA) receptor antibody encephalitis had not been reported in South Korea.1 In this study, we report a very rare case of a female with anti-NMDA receptor encephalitis that would be triggered by BNT162b2 m-RNA COVID-19 vaccination and, simultaneously, detected with ovarian teratoma.
Case Report
A 20-year-old female patient presented with the chief complaint of convulsive movement. She received first dose of the BNT162b2 COVID-19 m-RNA vaccine 3 days before admission. The day after vaccination, she showed abnormal behavior that began repetitively asking the same questions and sent inappropriate text messages to friends. On post-vaccination day 2, she showed disturbances of comprehension and reading. In the morning of admission day, she showed convulsive seizure that was sustained for 2 minutes with head version to the left side and upper eye version. On arrival, she was unable to remember the seizure event and to recognize the reason why she came to emergency room.
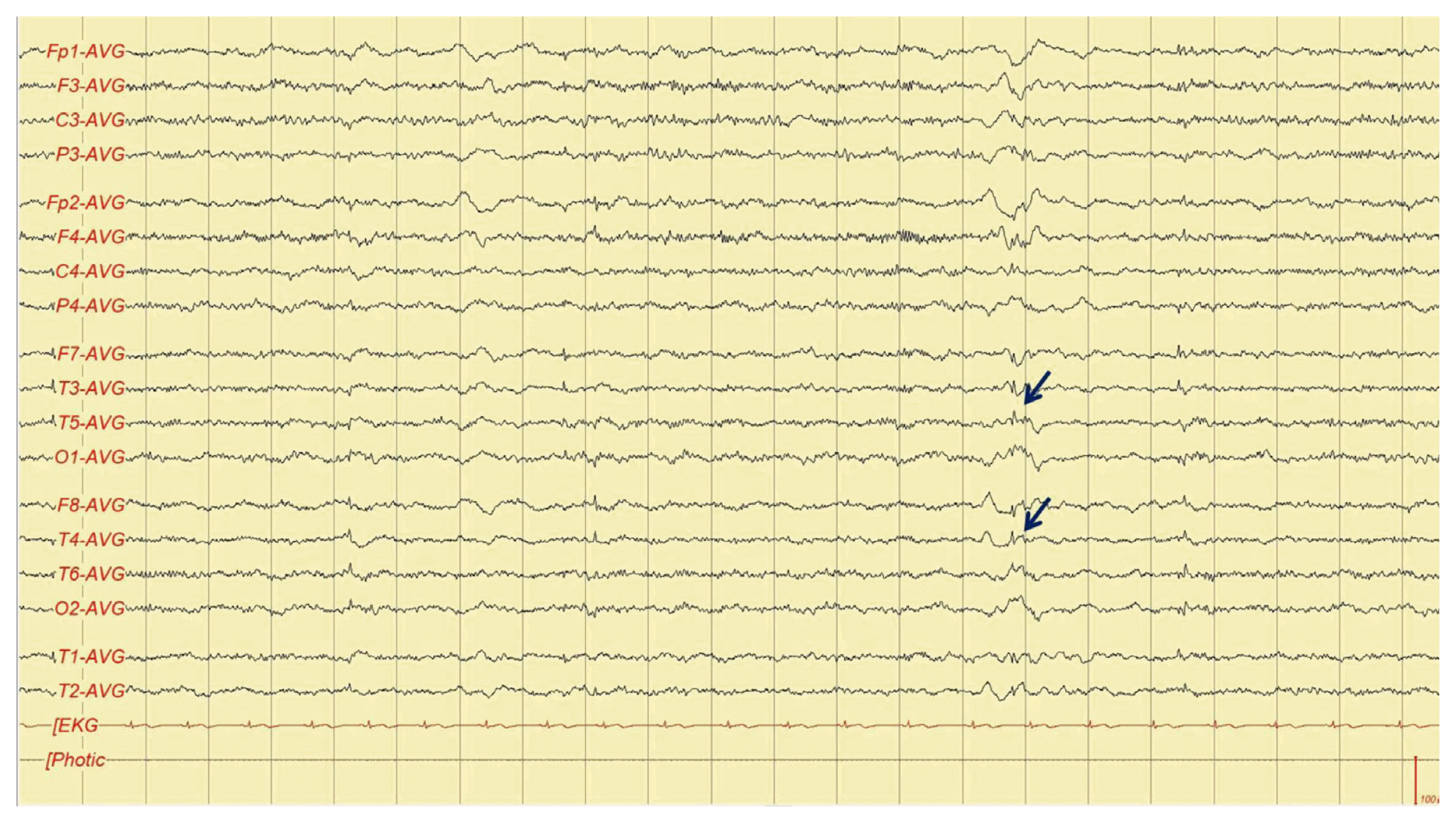
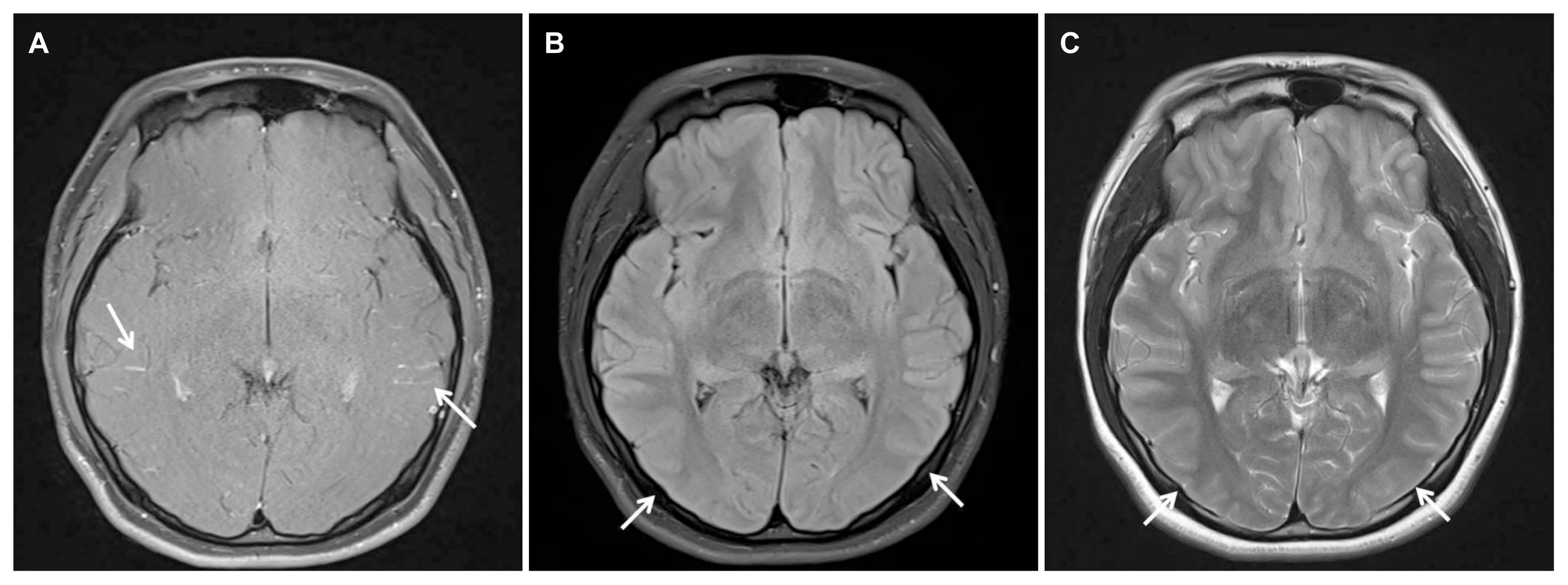
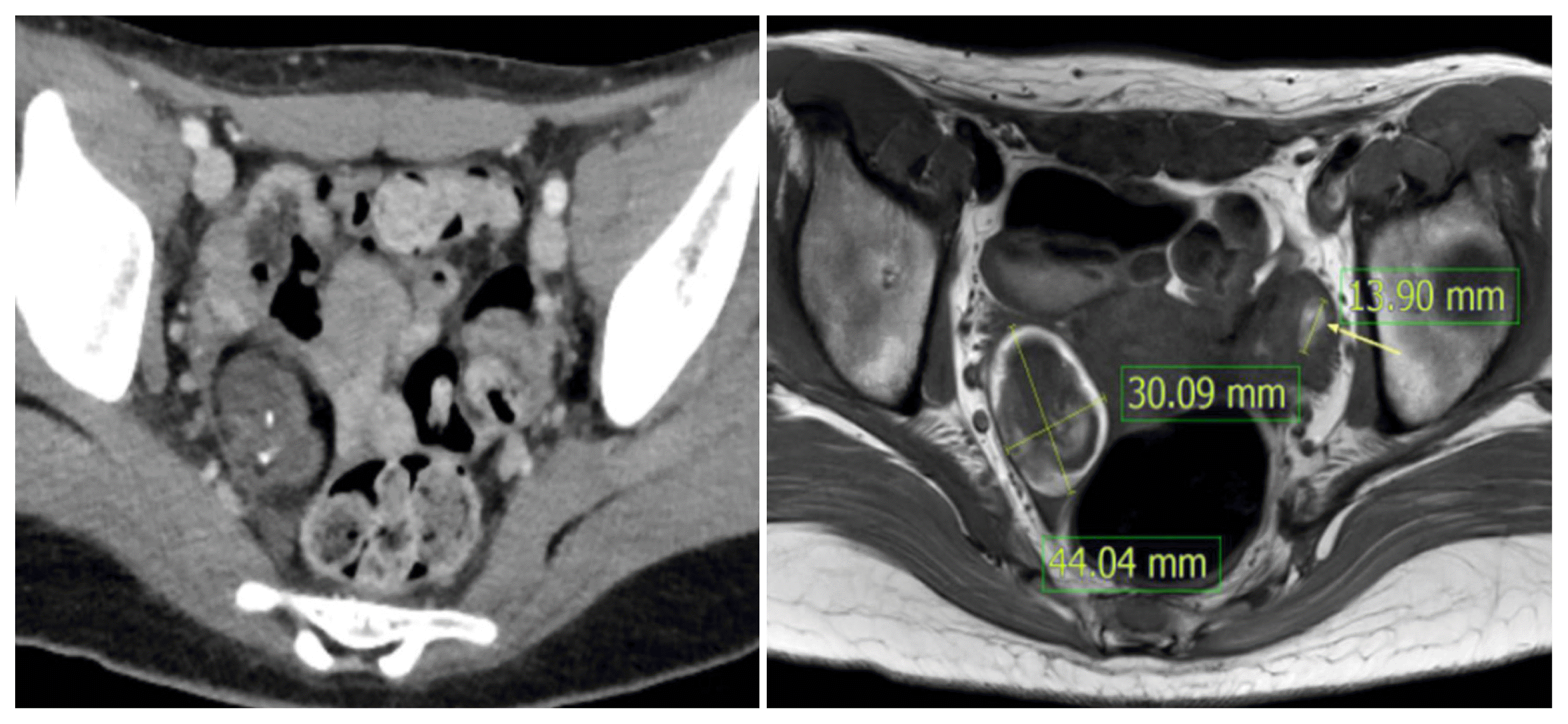
An electroencephalogram showed frequent spike-and-waves in the bilateral temporal areas (Fig. 1). Structural magnetic resonance imaging (MRI) of her brain was normal except leptomeningeal enhancement and gyral swelling in both cerebral convexity on T1-weighted contrast-enhanced image and subtle signal change on T2-weighted and fluid attenuated inversion recovery image (Fig. 2). Cerebrospinal fluid (CSF) studies revealed pleocytosis (58 white blood cells/mm3, lymphocyte dominant) and mild elevation of protein (42.7 mg/dL). Thyroid function test and autoantibody tests including rheumatoid factor, protein C, S, anti-double-stranded DNA antibody, anti-SSA/SSB antibody, anti-Smith antibody were performed which showed no significant abnormality. Deducing herpes simplex virus encephalitis, we administered acyclovir (10 mg/kg IV 3 days) for 9 days, but symptoms had worsened. Serum varicella zoster virus (VZV) immunoglobulin (Ig) G antibody was positive, but VZV IgM antibody and polymerized chain reaction were negative. Anti-NMDA receptor antibodies were identified in both serum and CSF. She was treated with methylprednisolone (1.0 g/day for 5 days) and intravenous immunoglobulin (0.4 g/Kg/d for 5 days), which showed no significant improvement. Bilateral ovarian teratoma was revealed on pelvic computed tomography (CT) and MRI (Fig. 3). After treatment with rituximab and removal of teratoma, her neurological and psychiatric symptoms improved. She returned to usual life and, furthermore, had not experienced any symptoms.
Discussion
Anti-NMDA receptor encephalitis is an autoimmune disorder related to inflammation by antibodies to the NR 1 subunit of the NMDA receptor.2 The symptom of this disease is known as multistage illness progression that initiate from psychiatric symptoms to seizure, memory disturbances and dyskinesia.3–5 It affects more females than males and is associated with viral infection, vaccination, or tumor.4
Some cases were reported about relation between this disease and vaccination such as tetanus/diphtheria/pertussis and polio vaccines and H1N1 vaccine.3,6 A previous study presented the case of young woman who diagnosed with anti-NMDA receptor encephalitis after receiving a tetanus, diphtheria, pertussis, polio vaccine booster dose. They proposed that preexisting specific T- and B-lymphocytes that produce anti-NMDA receptor antibodies were re-stimulated by vaccination and it leaded to excessive antibody synthesis.7 The present case presented with anti-NMDA receptor antibody encephalitis after vaccination with BNT162b2 m-RNA COVID 19. Further evaluation also revealed ovarian teratoma.
We hypothesize that Anti-NMDA receptor antibodies that were present before vaccination could be activated by BNT162b2 COVID-19 vaccine. If COVID-19 vaccine recipient shows neuro-psychiatric symptoms with seizure, diagnostic work-up should include anti-NMDA receptor antibodies and radiologic evaluation such as pelvic CT to reveal ovarian teratoma. Our hypothesis may be hasty because there is no previous report to support it. Further research is needed to elucidate the association between COVID-19 vaccination and anti-NMDA receptor encephalitis